How To Deal With Pes Planus
Overview

Pes planus is a condition in which the arch or instep of the foot collapses and comes in contact with the ground. In some individuals, this arch never develops while they are growing. Alternative names include pes planovalgus, flat feet, fallen arches, pronation of the feet.
Causes
Flat feet in adults can appear for a number of reasons. Arches never developed properly. Damage to the tendons that support the arch. Damage or inflammation of the posterior tibial tendon which runs from your lower leg, down and across your ankle, and connects to the middle of the arch. Trauma involving broken bones in the foot. Rheumatoid arthritis. Aging, pregnancy, nerve damage, obesity or even diabetes.
Symptoms
It?s possible to have fallen arches and experience no symptoms whatsoever. But many people do notice some problems with this condition. Their feet, back and legs ache. Standing on their toes is difficult, if not impossible, and they note swelling around the arch and heel.
Diagnosis
Diagnosis of flat feet or fallen arches can be made by your health practitioner and is based on the following. Clinical assessment involving visual gait assessment, as well as biomechanical assessment. A detailed family and medical history. A pain history assessment determining the location of painful symptoms. Physical palpation of the feet and painful areas. Imaging such as MRI or x-ray can be used by your practitioner to assist in the diagnosis.
best arch support insoles for plantar fasciitis
Non Surgical Treatment
Custom orthotics are specially designed insoles, which are made for your by prescription. This is done by taking a plaster cast of the foot in its neutral position and is then sent to a laboratory, with your prescription to be made to your exact specifications. The insole then correctly aligns your foot and as a result your body. This will relieve abnormal strain of tissues and structures which can cause pain. For less severe mal-alignments or for sports use a wide variety of temporary insoles.
Surgical Treatment
Surgery is typically offered as a last resort in people with significant pain that is resistant to other therapies. The treatment of a rigid flatfoot depends on its cause. Congenital vertical talus. Your doctor may suggest a trial of serial casting. The foot is placed in a cast and the cast is changed frequently to reposition the foot gradually. However, this generally has a low success rate. Most people ultimately need surgery to correct the problem. Tarsal coalition. Treatment depends on your age, extent of bone fusion and severity of symptoms. For milder cases, your doctor may recommend nonsurgical treatment with shoe inserts, wrapping of the foot with supportive straps or temporarily immobilizing the foot in a cast. For more severe cases, surgery is necessary to relieve pain and improve the flexibility of the foot. Lateral subtalar dislocation. The goal is to move the dislocated bone back into place as soon as possible. If there is no open wound, the doctor may push the bone back into proper alignment without making an incision. Anesthesia is usually given before this treatment. Once this is accomplished, a short leg cast must be worn for about four weeks to help stabilize the joint permanently. About 15% to 20% of people with lateral subtalar dislocation must be treated with surgery to reposition the dislocated bone.
Prevention
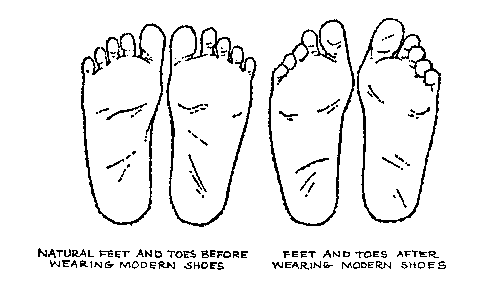
Flatfeet in children are often an inherited family trait, but it may be possible to prevent the condition in some cases. Recent research has shown that there are several social or cultural factors that can cause flatfeet. These factors include the following, obesity, overweight, unnecessary orthopedic treatments, wearing rigid shoes at a young age, In 1992, a study in India of 2300 children aged 4-13 demonstrated a significant difference in the rate of flatfeet among those who wore shoes regularly and those who did not. In this study, wearing inflexible, closed-toe shoes in early childhood was shown to have a negative effect on the normal development of arches. Children who were allowed to go barefoot or who wore light sandals and slippers had a much lower rate of flatfeet. In 1999, a study in Spain of 1181 children aged 4-13 revealed that the use of orthopedic shoes for treatment of flatfeet in children not only failed to correct the problem, but actually worsened the condition by preventing the normal flexing and arch development of bare or lightly protected feet. Finally, in 2006, a study of 835 children aged 3-6 showed significant differences in the rate of flatfeet based on weight, with normal-weight children having lower rates of flatfeet than children who were overweight or obese. Among adults, flatfeet due to injury, disease, or normal aging are not preventable. However, when flatfeet are related to lifestyle factors, such as physical activities, shoe selection, and weight gain, careful attention to these factors may prevent the development of flatfeet.

Pes planus is a condition in which the arch or instep of the foot collapses and comes in contact with the ground. In some individuals, this arch never develops while they are growing. Alternative names include pes planovalgus, flat feet, fallen arches, pronation of the feet.
Causes
Flat feet in adults can appear for a number of reasons. Arches never developed properly. Damage to the tendons that support the arch. Damage or inflammation of the posterior tibial tendon which runs from your lower leg, down and across your ankle, and connects to the middle of the arch. Trauma involving broken bones in the foot. Rheumatoid arthritis. Aging, pregnancy, nerve damage, obesity or even diabetes.
Symptoms
It?s possible to have fallen arches and experience no symptoms whatsoever. But many people do notice some problems with this condition. Their feet, back and legs ache. Standing on their toes is difficult, if not impossible, and they note swelling around the arch and heel.
Diagnosis
Diagnosis of flat feet or fallen arches can be made by your health practitioner and is based on the following. Clinical assessment involving visual gait assessment, as well as biomechanical assessment. A detailed family and medical history. A pain history assessment determining the location of painful symptoms. Physical palpation of the feet and painful areas. Imaging such as MRI or x-ray can be used by your practitioner to assist in the diagnosis.
best arch support insoles for plantar fasciitis
Non Surgical Treatment
Custom orthotics are specially designed insoles, which are made for your by prescription. This is done by taking a plaster cast of the foot in its neutral position and is then sent to a laboratory, with your prescription to be made to your exact specifications. The insole then correctly aligns your foot and as a result your body. This will relieve abnormal strain of tissues and structures which can cause pain. For less severe mal-alignments or for sports use a wide variety of temporary insoles.
Surgical Treatment

Surgery is typically offered as a last resort in people with significant pain that is resistant to other therapies. The treatment of a rigid flatfoot depends on its cause. Congenital vertical talus. Your doctor may suggest a trial of serial casting. The foot is placed in a cast and the cast is changed frequently to reposition the foot gradually. However, this generally has a low success rate. Most people ultimately need surgery to correct the problem. Tarsal coalition. Treatment depends on your age, extent of bone fusion and severity of symptoms. For milder cases, your doctor may recommend nonsurgical treatment with shoe inserts, wrapping of the foot with supportive straps or temporarily immobilizing the foot in a cast. For more severe cases, surgery is necessary to relieve pain and improve the flexibility of the foot. Lateral subtalar dislocation. The goal is to move the dislocated bone back into place as soon as possible. If there is no open wound, the doctor may push the bone back into proper alignment without making an incision. Anesthesia is usually given before this treatment. Once this is accomplished, a short leg cast must be worn for about four weeks to help stabilize the joint permanently. About 15% to 20% of people with lateral subtalar dislocation must be treated with surgery to reposition the dislocated bone.
Prevention
Flatfeet in children are often an inherited family trait, but it may be possible to prevent the condition in some cases. Recent research has shown that there are several social or cultural factors that can cause flatfeet. These factors include the following, obesity, overweight, unnecessary orthopedic treatments, wearing rigid shoes at a young age, In 1992, a study in India of 2300 children aged 4-13 demonstrated a significant difference in the rate of flatfeet among those who wore shoes regularly and those who did not. In this study, wearing inflexible, closed-toe shoes in early childhood was shown to have a negative effect on the normal development of arches. Children who were allowed to go barefoot or who wore light sandals and slippers had a much lower rate of flatfeet. In 1999, a study in Spain of 1181 children aged 4-13 revealed that the use of orthopedic shoes for treatment of flatfeet in children not only failed to correct the problem, but actually worsened the condition by preventing the normal flexing and arch development of bare or lightly protected feet. Finally, in 2006, a study of 835 children aged 3-6 showed significant differences in the rate of flatfeet based on weight, with normal-weight children having lower rates of flatfeet than children who were overweight or obese. Among adults, flatfeet due to injury, disease, or normal aging are not preventable. However, when flatfeet are related to lifestyle factors, such as physical activities, shoe selection, and weight gain, careful attention to these factors may prevent the development of flatfeet.
All The Things You Will Need To Know About Heel Ache
Overview
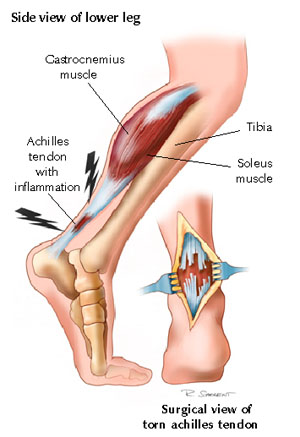
Your foot is made up of 26 bones, 33 joints, and more than 100 tendons. The heel is the largest bone in your foot. If you overuse or injure your heel, you may experience heel pain. This can range from mild to disabling. In many cases, if you have heel pain, you will need a doctor to diagnose the cause.
Causes
Plantar fasciitis can come from a number of underlying causes. Finding the precise reason for the heel pain is sometimes difficult. As you can imagine, when the foot is on the ground a tremendous amount of force (the full weight of the body) is concentrated on the plantar fascia. This force stretches the plantar fascia as the arch of the foot tries to flatten from the weight of your body. This is just how the string on a bow is stretched by the force of the bow trying to straighten. This leads to stress on the plantar fascia where it attaches to the heel bone. Small tears of the fascia can result. These tears are normally repaired by the body. As this process of injury and repair repeats itself over and over again, a bone spur (a pointed outgrowth of the bone) sometimes forms as the body's response to try to firmly attach the fascia to the heelbone. This appears on an X-ray of the foot as a heel spur. Bone spurs occur along with plantar fasciitis but they are not the cause of the problem. As we age, the very important fat pad that makes up the fleshy portion of the heel becomes thinner and degenerates (starts to break down). This can lead to inadequate padding on the heel. With less of a protective pad on the heel, there is a reduced amount of shock absorption. These are additional factors that might lead to plantar fasciitis. Some physicians feel that the small nerves that travel under the plantar fascia on their way to the forefoot become irritated and may contribute to the pain. But some studies have been able to show that pain from compression of the nerve is different from plantar fasciitis pain. In many cases, the actual source of the painful heel may not be defined clearly. Other factors that may contribute to the development of plantar fasciitis include obesity, trauma, weak plantar flexor muscles, excessive foot pronation (flat foot) or other alignment problems in the foot and or ankle, and poor footwear.
Symptoms
Plantar fasciitis is a condition of irritation to the plantar fascia, the thick ligament on the bottom of your foot. It classically causes pain and stiffness on the bottom of your heel and feels worse in the morning with the first steps out of bed and also in the beginning of an activity after a period of rest. For instance, after driving a car, people feel pain when they first get out, or runners will feel discomfort for the first few minutes of their run. This occurs because the plantar fascia is not well supplied by blood, which makes this condition slow in healing, and a certain amount of activity is needed to get the area to warm up. Plantar fasciitis can occur for various reasons: use of improper, non-supportive shoes; over-training in sports; lack of flexibility; weight gain; prolonged standing; and, interestingly, prolonged bed rest.
Diagnosis
A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans.
Non Surgical Treatment
Once diagnosed, treatment for plantar fasciitis may include one or more of the following: advice on footwear, in particular use of arch-supportive footwear; avoid walking barefoot; stretching exercises, shoe modifications such as heel pads, taping and strapping, anti-inflammatories and orthotic devices to correct abnormal foot mechanics. Injection therapy with corticosteroids is only advisable if all the conservative treatment methods mentioned above have been exhausted due to undesired effects implicated with steroid infusion in the heels.
Surgical Treatment
Surgery is a last resort in the treatment of heel pain. Physicians have developed many procedures in the last 100 years to try to cure heel pain. Most procedures that are commonly used today focus on several areas, remove the bone spur (if one is present), release the plantar fascia (plantar fasciotomy), release pressure on the small nerves in the area. Usually the procedure is done through a small incision on the inside edge of the foot, although some surgeons now perform this type of surgery using an endoscope. An endoscope is a tiny TV camera that can be inserted into a joint or under the skin to allow the surgeon to see the structures involved in the surgery. By using the endoscope, a surgeon can complete the surgery with a smaller incision and presumably less damage to normal tissues. It is unclear whether an endoscopic procedure for this condition is better than the traditional small incision. Surgery usually involves identifying the area where the plantar fascia attaches to the heel and releasing the fascia partially from the bone. If a small spur is present this is removed. The small nerves that travel under the plantar fascia are identified and released from anything that seems to be causing pressure on the nerves. This surgery can usually be done on an outpatient basis. This means you can leave the hospital the same day.
heel bursitis
Prevention

Before you get out of bed in the morning, and then periodically throughout the day, do the following exercises to increase flexibility and ease pain. Slowly flex your foot and toes to stretch the tissue on the bottom of your sore foot. Hold the stretch for 10 counts. Relax and repeat. Do gentle ankle rolls to keep the tissues around the ankle and on the back of the heel flexible. Sit on the edge of your bed and roll your foot back and forth over a tennis ball.

Your foot is made up of 26 bones, 33 joints, and more than 100 tendons. The heel is the largest bone in your foot. If you overuse or injure your heel, you may experience heel pain. This can range from mild to disabling. In many cases, if you have heel pain, you will need a doctor to diagnose the cause.
Causes
Plantar fasciitis can come from a number of underlying causes. Finding the precise reason for the heel pain is sometimes difficult. As you can imagine, when the foot is on the ground a tremendous amount of force (the full weight of the body) is concentrated on the plantar fascia. This force stretches the plantar fascia as the arch of the foot tries to flatten from the weight of your body. This is just how the string on a bow is stretched by the force of the bow trying to straighten. This leads to stress on the plantar fascia where it attaches to the heel bone. Small tears of the fascia can result. These tears are normally repaired by the body. As this process of injury and repair repeats itself over and over again, a bone spur (a pointed outgrowth of the bone) sometimes forms as the body's response to try to firmly attach the fascia to the heelbone. This appears on an X-ray of the foot as a heel spur. Bone spurs occur along with plantar fasciitis but they are not the cause of the problem. As we age, the very important fat pad that makes up the fleshy portion of the heel becomes thinner and degenerates (starts to break down). This can lead to inadequate padding on the heel. With less of a protective pad on the heel, there is a reduced amount of shock absorption. These are additional factors that might lead to plantar fasciitis. Some physicians feel that the small nerves that travel under the plantar fascia on their way to the forefoot become irritated and may contribute to the pain. But some studies have been able to show that pain from compression of the nerve is different from plantar fasciitis pain. In many cases, the actual source of the painful heel may not be defined clearly. Other factors that may contribute to the development of plantar fasciitis include obesity, trauma, weak plantar flexor muscles, excessive foot pronation (flat foot) or other alignment problems in the foot and or ankle, and poor footwear.
Symptoms
Plantar fasciitis is a condition of irritation to the plantar fascia, the thick ligament on the bottom of your foot. It classically causes pain and stiffness on the bottom of your heel and feels worse in the morning with the first steps out of bed and also in the beginning of an activity after a period of rest. For instance, after driving a car, people feel pain when they first get out, or runners will feel discomfort for the first few minutes of their run. This occurs because the plantar fascia is not well supplied by blood, which makes this condition slow in healing, and a certain amount of activity is needed to get the area to warm up. Plantar fasciitis can occur for various reasons: use of improper, non-supportive shoes; over-training in sports; lack of flexibility; weight gain; prolonged standing; and, interestingly, prolonged bed rest.
Diagnosis
A podiatrist (doctor who specializes in the evaluation and treatment of foot diseases) will carry out a physical examination, and ask pertinent questions about the pain. The doctor will also ask the patient how much walking and standing the patient does, what type of footwear is worn, and details of the his/her medical history. Often this is enough to make a diagnosis. Sometimes further diagnostic tests are needed, such as blood tests and imaging scans.
Non Surgical Treatment
Once diagnosed, treatment for plantar fasciitis may include one or more of the following: advice on footwear, in particular use of arch-supportive footwear; avoid walking barefoot; stretching exercises, shoe modifications such as heel pads, taping and strapping, anti-inflammatories and orthotic devices to correct abnormal foot mechanics. Injection therapy with corticosteroids is only advisable if all the conservative treatment methods mentioned above have been exhausted due to undesired effects implicated with steroid infusion in the heels.
Surgical Treatment
Surgery is a last resort in the treatment of heel pain. Physicians have developed many procedures in the last 100 years to try to cure heel pain. Most procedures that are commonly used today focus on several areas, remove the bone spur (if one is present), release the plantar fascia (plantar fasciotomy), release pressure on the small nerves in the area. Usually the procedure is done through a small incision on the inside edge of the foot, although some surgeons now perform this type of surgery using an endoscope. An endoscope is a tiny TV camera that can be inserted into a joint or under the skin to allow the surgeon to see the structures involved in the surgery. By using the endoscope, a surgeon can complete the surgery with a smaller incision and presumably less damage to normal tissues. It is unclear whether an endoscopic procedure for this condition is better than the traditional small incision. Surgery usually involves identifying the area where the plantar fascia attaches to the heel and releasing the fascia partially from the bone. If a small spur is present this is removed. The small nerves that travel under the plantar fascia are identified and released from anything that seems to be causing pressure on the nerves. This surgery can usually be done on an outpatient basis. This means you can leave the hospital the same day.
heel bursitis
Prevention

Before you get out of bed in the morning, and then periodically throughout the day, do the following exercises to increase flexibility and ease pain. Slowly flex your foot and toes to stretch the tissue on the bottom of your sore foot. Hold the stretch for 10 counts. Relax and repeat. Do gentle ankle rolls to keep the tissues around the ankle and on the back of the heel flexible. Sit on the edge of your bed and roll your foot back and forth over a tennis ball.
How To Measure Leg Length Discrepancy
Overview
A difference in the length of your lower and/or upper legs is called a leg length discrepancy. This is fairly common, actually. One study reported that 32 percent of 600 individuals had a difference in their leg lengths ranging from one-fifth to three-fifths of an inch. A person might not even notice if one leg is slightly longer than the other. However, if the difference is not minimal, treatment may be required.
Causes
An anatomical short leg is due to several orthopedic or medical condition mechanisms. Often, one leg simply stops growing before the other one does and is called ?congenital?. We often see mother-daughters or father-sons who exhibit virtually the same degree of shortness on the same side. Often it is not known why this occurs, but it seems to account for approximately 25% of the population demonstrating a true LLD. Other causes of a true LLD include trauma or broken bones, surgical repair, joint replacement, radiation exposure, tumors or Legg-Calves-Perthes disease.
Symptoms
Often there are few or no symptoms prior to the age of 25-35. The most common symptom is chronic lower back pain, but also is frequently middle and upper back pain. Same-sided and repeated injury or pain to the hip, knee and/or ankle is also a hallmark of a long-standing untreated LLD. It is not uncommon to have buttock or radiating hip pain that is non-dermatomal (not from a disc) and tends to go away when lying down.
Diagnosis
On standing examination one iliac crest may be higher/lower than the other. However a physiotherapist, osteopath or chiropractor will examine the LLD in prone or supine position and measure it, confirming the diagnosis of structural (or functional) LLD. The LLD should be measured using bony fixed points. X-Ray should be taken in a standing position. The osteopath, physiotherapist or chiropractor will look at femoral head & acetabulum, knee joints, ankle joints.
Non Surgical Treatment
Internal heel lifts: Putting a simple heel lift inside the shoe or onto a foot orthotic has the advantage of being transferable to many pairs of shoes. It is also aesthetically more pleasing as the lift remains hidden from view. However, there is a limit as to how high the lift can be before affecting shoe fit. Dress shoes will usually only accommodate small lifts (1/8"1/4") before the heel starts to piston out of the shoe. Sneakers and workboots may allow higher lifts, e.g., up to 1/2", before heel slippage problems arise. External heel lifts: If a lift of greater than 1/2" is required, you should consider adding to the outsole of the shoe. In this way, the shoe fit remains good. Although some patients may worry about the cosmetics of the shoe, it does ensure better overall function. Nowadays with the development of synthetic foams and crepes, such lifts do not have to be as heavy as the cork buildups of the past. External buildups are not transferable and they will wear down over time, so the patient will need to be vigilant in having them repaired. On ladies' high-heel shoes, it may be possible to lower one heel and thereby correct the imbalance.

can you stretch to get taller?
Surgical Treatment
Bone growth restriction (epiphysiodesis) The objective of this surgical procedure is to slow down growth in the longer leg. During surgery, doctors alter the growth plate of the bone in the longer leg by inserting a small plate or staples. This slows down growth, allowing the shorter leg to catch up over time. Your child may spend a night in the hospital after this procedure or go home the same day. Doctors may place a knee brace on the leg for a few days. It typically takes 2 to 3 months for the leg to heal completely. An alternative approach involves lengthening the shorter bone. We are more likely to recommend this approach if your child is on the short side of the height spectrum.
A difference in the length of your lower and/or upper legs is called a leg length discrepancy. This is fairly common, actually. One study reported that 32 percent of 600 individuals had a difference in their leg lengths ranging from one-fifth to three-fifths of an inch. A person might not even notice if one leg is slightly longer than the other. However, if the difference is not minimal, treatment may be required.

Causes
An anatomical short leg is due to several orthopedic or medical condition mechanisms. Often, one leg simply stops growing before the other one does and is called ?congenital?. We often see mother-daughters or father-sons who exhibit virtually the same degree of shortness on the same side. Often it is not known why this occurs, but it seems to account for approximately 25% of the population demonstrating a true LLD. Other causes of a true LLD include trauma or broken bones, surgical repair, joint replacement, radiation exposure, tumors or Legg-Calves-Perthes disease.
Symptoms
Often there are few or no symptoms prior to the age of 25-35. The most common symptom is chronic lower back pain, but also is frequently middle and upper back pain. Same-sided and repeated injury or pain to the hip, knee and/or ankle is also a hallmark of a long-standing untreated LLD. It is not uncommon to have buttock or radiating hip pain that is non-dermatomal (not from a disc) and tends to go away when lying down.
Diagnosis
On standing examination one iliac crest may be higher/lower than the other. However a physiotherapist, osteopath or chiropractor will examine the LLD in prone or supine position and measure it, confirming the diagnosis of structural (or functional) LLD. The LLD should be measured using bony fixed points. X-Ray should be taken in a standing position. The osteopath, physiotherapist or chiropractor will look at femoral head & acetabulum, knee joints, ankle joints.
Non Surgical Treatment
Internal heel lifts: Putting a simple heel lift inside the shoe or onto a foot orthotic has the advantage of being transferable to many pairs of shoes. It is also aesthetically more pleasing as the lift remains hidden from view. However, there is a limit as to how high the lift can be before affecting shoe fit. Dress shoes will usually only accommodate small lifts (1/8"1/4") before the heel starts to piston out of the shoe. Sneakers and workboots may allow higher lifts, e.g., up to 1/2", before heel slippage problems arise. External heel lifts: If a lift of greater than 1/2" is required, you should consider adding to the outsole of the shoe. In this way, the shoe fit remains good. Although some patients may worry about the cosmetics of the shoe, it does ensure better overall function. Nowadays with the development of synthetic foams and crepes, such lifts do not have to be as heavy as the cork buildups of the past. External buildups are not transferable and they will wear down over time, so the patient will need to be vigilant in having them repaired. On ladies' high-heel shoes, it may be possible to lower one heel and thereby correct the imbalance.

can you stretch to get taller?
Surgical Treatment
Bone growth restriction (epiphysiodesis) The objective of this surgical procedure is to slow down growth in the longer leg. During surgery, doctors alter the growth plate of the bone in the longer leg by inserting a small plate or staples. This slows down growth, allowing the shorter leg to catch up over time. Your child may spend a night in the hospital after this procedure or go home the same day. Doctors may place a knee brace on the leg for a few days. It typically takes 2 to 3 months for the leg to heal completely. An alternative approach involves lengthening the shorter bone. We are more likely to recommend this approach if your child is on the short side of the height spectrum.
Mortons Neuroma Treatment
Overview
 Morton neuroma (interdigital neuroma), first described in 1876, is a perineural fibrosis and nerve degeneration of the common digital nerve. Morton neuroma, or Morton's neuroma, is not a true neuroma, although it results in neuropathic pain in the distribution of the interdigital nerve secondary to repetitive irritation of the nerve. The most frequent location is between the third and fourth metatarsals (third webspace). Other, less common locations are between the second and third metatarsals (second webspace) and, rarely, between the first and second (first webspace) or fourth and fifth (fourth webspace) metatarsals.
Morton neuroma (interdigital neuroma), first described in 1876, is a perineural fibrosis and nerve degeneration of the common digital nerve. Morton neuroma, or Morton's neuroma, is not a true neuroma, although it results in neuropathic pain in the distribution of the interdigital nerve secondary to repetitive irritation of the nerve. The most frequent location is between the third and fourth metatarsals (third webspace). Other, less common locations are between the second and third metatarsals (second webspace) and, rarely, between the first and second (first webspace) or fourth and fifth (fourth webspace) metatarsals.
Causes
The exact cause of Morton?s neuroma is not known, but the choice of footwear seems be a factor. Wearing high heels (shoes with heels over 2 inches) can put extra pressure on the balls of the feet. Wearing tight or pointed toed shoes may squeeze the toes together or otherwise constrict their movement. For that reason, women are about 8 to 10 times more likely to develop Morton?s neuroma compared with men. People who are born with flat feet, high arches, or an abnormal position of the toes are more prone to developing Morton?s neuroma. This may be due to instability around the toe joints. Certain conditions that develop over time, such as bunions or hammer toes, are also associated with Morton?s neuroma. Some sports that involve running, including tennis and other racquet sports, can also increase the chance of developing Morton?s neuroma due to trauma or injury to the foot.
Symptoms
Neuroma patients occasionally complain of a ?pins and needles? sensation that spreads through their feet, or of a feeling akin to hitting their ?funny bone.? The sensation may be described as similar to an electric shock. Some patients also say that these symptoms, as well as those listed above, will come and go, depending on what they are wearing on their feet, the activity they are doing, or on other external factors.
Diagnosis
The diagnosis of interdigital neuroma is usually made by physical examination and review of the patient's medical history.MRI ad High Definition Ultrasound examination may be useful to confirm the diagnoses however they may still not be 100% reliable. The commonest reason for this is de to natural substances present in between the metatarsal heads and between the fat pad and the intermetatarsal ligament. These natural substances i.e. bursa, fat, capsular thickening and even bony growths, can all be a factor in the impingement process and may need to be surgically cleared.
Non Surgical Treatment
In most cases, initial treatment for this condition consists of padding and taping to disperse weight away from the neuroma. If the patient has flatfeet, an arch support is incorporated into footwear. The patient is instructed to wear shoes with wide toe boxes and avoid shoes with high heels. An injection of local anesthetic to relieve pain and a corticosteroid to reduce inflammation may be administered. The patient is advised to return in a week or 2 to monitor progress. If the pain has been relieved, the neuroma is probably small and caused by the structure of the patient's foot and the type of shoes the patient wears. It can be relieved by a custom-fitted orthotic that helps maintain the foot in a better position. Another type of therapy that may be used is alcohol sclerosing injections. In this treatment, the doctor injects a small amount of alcohol in the area of the neuroma area to help harden (sclerose) the nerve and relieve the pain. Injections are given every 7-10 days and, in many cases, 4-7 injections are needed for maximum relief. Please ask your physician for more information regarding this type of treatment.
Surgical Treatment
Surgery to remove the neuroma may be recommended if more conservative treatment does not solve the problem. While surgery usually relieves or completely removes the symptoms, it often leaves a permanent numb feeling at the site of the neuroma.
 Morton neuroma (interdigital neuroma), first described in 1876, is a perineural fibrosis and nerve degeneration of the common digital nerve. Morton neuroma, or Morton's neuroma, is not a true neuroma, although it results in neuropathic pain in the distribution of the interdigital nerve secondary to repetitive irritation of the nerve. The most frequent location is between the third and fourth metatarsals (third webspace). Other, less common locations are between the second and third metatarsals (second webspace) and, rarely, between the first and second (first webspace) or fourth and fifth (fourth webspace) metatarsals.
Morton neuroma (interdigital neuroma), first described in 1876, is a perineural fibrosis and nerve degeneration of the common digital nerve. Morton neuroma, or Morton's neuroma, is not a true neuroma, although it results in neuropathic pain in the distribution of the interdigital nerve secondary to repetitive irritation of the nerve. The most frequent location is between the third and fourth metatarsals (third webspace). Other, less common locations are between the second and third metatarsals (second webspace) and, rarely, between the first and second (first webspace) or fourth and fifth (fourth webspace) metatarsals.Causes
The exact cause of Morton?s neuroma is not known, but the choice of footwear seems be a factor. Wearing high heels (shoes with heels over 2 inches) can put extra pressure on the balls of the feet. Wearing tight or pointed toed shoes may squeeze the toes together or otherwise constrict their movement. For that reason, women are about 8 to 10 times more likely to develop Morton?s neuroma compared with men. People who are born with flat feet, high arches, or an abnormal position of the toes are more prone to developing Morton?s neuroma. This may be due to instability around the toe joints. Certain conditions that develop over time, such as bunions or hammer toes, are also associated with Morton?s neuroma. Some sports that involve running, including tennis and other racquet sports, can also increase the chance of developing Morton?s neuroma due to trauma or injury to the foot.
Symptoms
Neuroma patients occasionally complain of a ?pins and needles? sensation that spreads through their feet, or of a feeling akin to hitting their ?funny bone.? The sensation may be described as similar to an electric shock. Some patients also say that these symptoms, as well as those listed above, will come and go, depending on what they are wearing on their feet, the activity they are doing, or on other external factors.
Diagnosis
The diagnosis of interdigital neuroma is usually made by physical examination and review of the patient's medical history.MRI ad High Definition Ultrasound examination may be useful to confirm the diagnoses however they may still not be 100% reliable. The commonest reason for this is de to natural substances present in between the metatarsal heads and between the fat pad and the intermetatarsal ligament. These natural substances i.e. bursa, fat, capsular thickening and even bony growths, can all be a factor in the impingement process and may need to be surgically cleared.
Non Surgical Treatment
In most cases, initial treatment for this condition consists of padding and taping to disperse weight away from the neuroma. If the patient has flatfeet, an arch support is incorporated into footwear. The patient is instructed to wear shoes with wide toe boxes and avoid shoes with high heels. An injection of local anesthetic to relieve pain and a corticosteroid to reduce inflammation may be administered. The patient is advised to return in a week or 2 to monitor progress. If the pain has been relieved, the neuroma is probably small and caused by the structure of the patient's foot and the type of shoes the patient wears. It can be relieved by a custom-fitted orthotic that helps maintain the foot in a better position. Another type of therapy that may be used is alcohol sclerosing injections. In this treatment, the doctor injects a small amount of alcohol in the area of the neuroma area to help harden (sclerose) the nerve and relieve the pain. Injections are given every 7-10 days and, in many cases, 4-7 injections are needed for maximum relief. Please ask your physician for more information regarding this type of treatment.

Surgical Treatment
Surgery to remove the neuroma may be recommended if more conservative treatment does not solve the problem. While surgery usually relieves or completely removes the symptoms, it often leaves a permanent numb feeling at the site of the neuroma.
Shoe Lifts The Podiatrists Solution For Leg Length Difference
There are actually not one but two unique variations of leg length discrepancies, congenital and acquired. Congenital implies you are born with it. One leg is anatomically shorter in comparison to the other. Through developmental periods of aging, the human brain picks up on the walking pattern and recognizes some variation. Your body usually adapts by tilting one shoulder to the "short" side. A difference of less than a quarter inch is not very irregular, does not need Shoe Lifts to compensate and usually does not have a serious effect over a lifetime.

Leg length inequality goes mainly undiscovered on a daily basis, yet this problem is easily remedied, and can eliminate numerous incidents of back problems.
Therapy for leg length inequality typically involves Shoe Lifts . Many are very reasonably priced, generally being below twenty dollars, in comparison to a custom orthotic of $200 if not more. Differences over a quarter inch can take their toll on the spine and should probably be compensated for with a heel lift. In some cases, the shortage can be so extreme that it requires a full lift to both the heel and sole of the shoe.
Mid back pain is the most widespread health problem impacting people today. Over 80 million men and women suffer from back pain at some point in their life. It's a problem which costs businesses millions each year on account of lost time and production. Innovative and improved treatment solutions are always sought after in the hope of reducing the economical impact this condition causes.

People from all corners of the earth suffer the pain of foot ache due to leg length discrepancy. In a lot of these situations Shoe Lifts might be of very helpful. The lifts are capable of decreasing any discomfort and pain in the feet. Shoe Lifts are recommended by many professional orthopaedic orthopedists.
So that you can support the human body in a balanced manner, your feet have got a very important task to play. Inspite of that, it is sometimes the most neglected area in the human body. Some people have flat-feet which means there may be unequal force placed on the feet. This will cause other parts of the body like knees, ankles and backs to be impacted too. Shoe Lifts make sure that ideal posture and balance are restored.

Leg length inequality goes mainly undiscovered on a daily basis, yet this problem is easily remedied, and can eliminate numerous incidents of back problems.
Therapy for leg length inequality typically involves Shoe Lifts . Many are very reasonably priced, generally being below twenty dollars, in comparison to a custom orthotic of $200 if not more. Differences over a quarter inch can take their toll on the spine and should probably be compensated for with a heel lift. In some cases, the shortage can be so extreme that it requires a full lift to both the heel and sole of the shoe.
Mid back pain is the most widespread health problem impacting people today. Over 80 million men and women suffer from back pain at some point in their life. It's a problem which costs businesses millions each year on account of lost time and production. Innovative and improved treatment solutions are always sought after in the hope of reducing the economical impact this condition causes.

People from all corners of the earth suffer the pain of foot ache due to leg length discrepancy. In a lot of these situations Shoe Lifts might be of very helpful. The lifts are capable of decreasing any discomfort and pain in the feet. Shoe Lifts are recommended by many professional orthopaedic orthopedists.
So that you can support the human body in a balanced manner, your feet have got a very important task to play. Inspite of that, it is sometimes the most neglected area in the human body. Some people have flat-feet which means there may be unequal force placed on the feet. This will cause other parts of the body like knees, ankles and backs to be impacted too. Shoe Lifts make sure that ideal posture and balance are restored.
Does A Calcaneal Spur Hurt?

Overview
A heel spur occurs when calcium deposits build up on the underside of the heel bone, a process that usually occurs over a period of many months. Heel spurs are often caused by strains on foot muscles and ligaments, stretching of the plantar fascia, and repeated tearing of the membrane that covers the heel bone. Heel spurs are especially common among athletes whose activities include large amounts of running and jumping. Heel spurs often cause no symptoms but can be associated with intermittent pain, especially while walking, jogging, or running. Sharp pain in the heel can also be experienced when standing after sitting for a long period of time. Heel spurs can be a result of plantar fasciitis.
Causes
Bone spurs can form anywhere in the feet in response to tight ligaments, repetitive stress injuries (typically from sports), obesity, even poorly fitting shoes. For instance, when the plantar fascia on the bottom of the foot pulls repeatedly on the heel, the ligament becomes inflamed, causing plantar fasciitis. As the bone tries to mend itself, a bone spur forms on the bottom of the heel, typically referred to as a heel spur. This is a common source of heel pain.

Symptoms
It is important to be aware that heel spurs may or may not cause symptoms. Symptoms are usually related to the plantar fasciitis. You may experience significant pain and it may be worse in the morning when you first wake up or during certain physical activities such as, walking, jogging, or running.
Diagnosis
A thorough history and physical exam is always necessary for the proper diagnosis of heel spurs and other foot conditions. X rays of the heel area are helpful, as excess bone production will be visible.
Non Surgical Treatment
Acupuncture and acupressure can used to address the pain of heel spurs, in addition to using friction massage to help break up scar tissue and delay the onset of bony formations. Physical therapy may help relieve pain and improve movement. The Feldenkrais method could be especially helpful for retraining some of the compensation movements caused by the pain from the spur. Guided imagery or a light massage on the foot may help to relieve some of the pain. Other treatments include low-gear cycling, and pool running. Some chiropractors approve of moderate use of aspirin or ibuprofen, or other appropriate anti-inflammatory drugs. Chiropractic manipulation is not recommended, although chiropractors may offer custom-fitted shoe orthotics and other allopathic-type treatments.
Surgical Treatment
When chronic heel pain fails to respond to conservative treatment, surgical treatment may be necessary. Heel surgery can provide relief of pain and restore mobility. The type of procedure used is based on examination and usually consists of releasing the excessive tightness of the plantar fascia, called a plantar fascia release. Depending on the presence of excess bony build up, the procedure may or may not include removal of heel spurs. Similar to other surgical interventions, there are various modifications and surgical enhancements regarding surgery of the heel.
Prevention
To prevent this condition, wearing properly fitted shoes with good arch support is very important. If a person is overweight, weight loss can help diminish stress on the feet and help prevent foot problems. For those who exercise frequently and intensely, proper stretching is always necessary, especially when there is an increase in activities or a change in running technique. It is not recommended to attempt to work through the pain, as this can change a mild case of heel spurs and plantar fascitis into a long-lasting and painful episode of the condition.
Does A Inferior Calcaneal Spur Hurt?

Overview
Heel Spurs should be called a traction spurs because they grow in the same direction that the tendons pull away from the heel bone, which is why it can occur on the bottom of the heel (Plantar Fasciitis) and on the back of the heel (Achilles Tendonitis). Some patients may only develop one type of heel spur, but both these problems are closely related so it's not unusual for a patient to have both heel spurs. It's important to note though that most heel spurs aren't the cause of your heel pain.
Causes
The plantar fascia is a thick, ligamentous connective tissue that runs from the calcaneus (heel bone) to the ball of the foot. This strong and tight tissue helps maintain the arch of the foot. It is also one of the major transmitters of weight across the foot as you walk or run. That's why tremendous stress is placed on the plantar fascia.

Symptoms
Symptoms may be similar to those of plantar fasciitis and include pain and tenderness at the base of the heel, pain on weight bearing and in severe cases difficulty walking. The main diagnosis of a heel spur is made by X-ray where a bony growth on the heel can be seen. A heel spur can occur without any symptoms at all and the athlete would never know they have the bony growth on the heel. Likewise, Plantar fasciitis can occur without the bone growth present.
Diagnosis
Diagnosis of a heel spur can be done with an x-ray, which will be able to reveal the bony spur. Normally, it occurs where the plantar fascia connects to the heel bone. When the plantar fascia ligament is pulled excessively it begins to pull away from the heel bone. When this excessive pulling occurs, it causes the body to respond by depositing calcium in the injured area, resulting in the formation of the bone spur. The Plantar fascia ligament is a fibrous band of connective tissue running between the heel bone and the ball of the foot. This structure maintains the arch of the foot and distributes weight along the foot as we walk. However, due to the stress that this ligament must endure, it can easily become damaged which commonly occurs along with heel spurs.
Non Surgical Treatment
The key for the proper treatment of heel spurs is determining what is causing the excessive stretching of the plantar fascia. When the cause is over-pronation (flat feet), an orthotic with rear foot posting and longitudinal arch support is an effective device to reduce the over-pronation, and allow the condition to heal. Other common treatments include stretching exercises, losing weight, wearing shoes that have a cushioned heel that absorbs shock, and elevating the heel with the use of a heel cradle, heel cup, or orthotic. Heel cradles and heel cups provide extra comfort and cushion to the heel, and reduce the amount of shock and shear forces experienced from everyday activities.
Surgical Treatment
Heel spur surgery should only be considered after less invasive treatment methods have been explored and ruled insufficient. The traditional surgical approach to treating heel spurs requires a scalpel cut to the bottom of the food which allows the surgeon to access the bone spur. Endoscopic plantar fasciotomies (EPF) involve one or two small incisions in the foot which allow the surgeon to access and operate on the bone spur endoscopically. Taking a surgical approach to heel spur treatment is a topic to explore with a foot and ankle specialist.
Prevention
A variety of steps can be taken to avoid heel pain and accompanying afflictions. Wear shoes that fit well-front, back, and sides-and have shock-absorbent soles, rigid shanks, and supportive heel counters. Wear the proper shoes for each activity. Do not wear shoes with excessive wear on heels or soles. Prepare properly before exercising. Warm up and do stretching exercises before and after running. Pace yourself when you participate in athletic activities. Don't underestimate your body's need for rest and good nutrition. If obese, lose weight.