Bursitis Of The Foot Problems
Whenever tissues rub against one another, a bursa forms to allow for smooth gliding. A bursa is a fluid-filled sac and occurs normally throughout the body. Only a few cell layers thick, a bursa is filled with a lubricating fluid. However, when irritated, a bursa can become markedly thickened and painful. This is often referred to as bursitis. The retrocalcaneal bursa is positioned to allow the Achilles tendon to glide over the back part (posterior aspect) of the heel bone. When this bone becomes enlarged, inflammation of the retrocalcaneal bursa occurs. This inflammation results in exquisite tenderness along the posterior aspect of the heel.
Causes
The calcaneal bursa can become inflamed in patients with heel spurs or in patients with poor-fitting shoes (eg, high heels). Inflammation can occur secondarily from Achilles tendinitis, especially in young athletes. Patients exhibit tenderness to palpation of the bursa anterior to the Achilles tendon on both the medial and lateral aspects. They have pain with movement, which is worsened with dorsiflexion.
Symptoms
Pain at the back of the heel, especially when running uphill. Pain may get worse when rising on the toes (standing on tiptoes). Tenderness at the back of heel. Swelling at the back of heel.
Diagnosis
Magnetic resonance imaging (MRI) may demonstrate bursal inflammation, but this modality probably does not offer much more information than that found by careful physical examination. Theoretically, MRI could help the physician to determine whether the inflammation is within the subcutaneous bursa, the subtendinous bursa, or even within the tendon itself, however, such testing is generally not necessary. Ultrasonography may be a potentially useful tool for diagnosing pathologies of the Achilles tendon.
Non Surgical Treatment
The underlying cause of the bursitis must be identified to prevent further reoccurrences. Failure to eliminate the cause will lead to future flare ups and a poor and slow recovery. Future occurrences can be prevented with the use of stretches and strengthening exercises which will help prevent the muscles from tightening up over the bursa, Pilates and yoga are very good for this providing the aggravating movements are avoided. Wearing joint supports such as knee pads or elbow supports may also reduce the likelihood of redeveloping bursitis.
Prevention
You may be able to prevent bursitis from happening or coming back. Continue your home treatment with rest, ice, pain relievers, and gentle exercises. When you are ready to try the activity that caused the pain, start slowly and do it for short periods or at a slower speed. Warm up before and stretch after the activity. Increase your activity slowly, and stop if it hurts. Use ice afterward to prevent pain and swelling. Change the way you do activities with repeated movements that may strain your muscles or joints. For example if using a certain tool has caused bursitis, start switching hands or change the grip size of your tool. If sitting for long periods has caused bursitis, get up and walk around every hour. If a certain sport is causing bursitis, consider taking lessons to learn proper techniques. Have an expert check your equipment to make sure it's well suited to your size, strength, and ability. If certain activities at work may be causing bursitis, talk to your human resources department about other ways of doing your job, equipment changes, or other job assignments. Protect your joints from pressure. Cushion knees or elbows on hard surfaces, and wear shoes that fit you well and have good support.
Do Hammertoe Straighteners Actually Work
 Overview
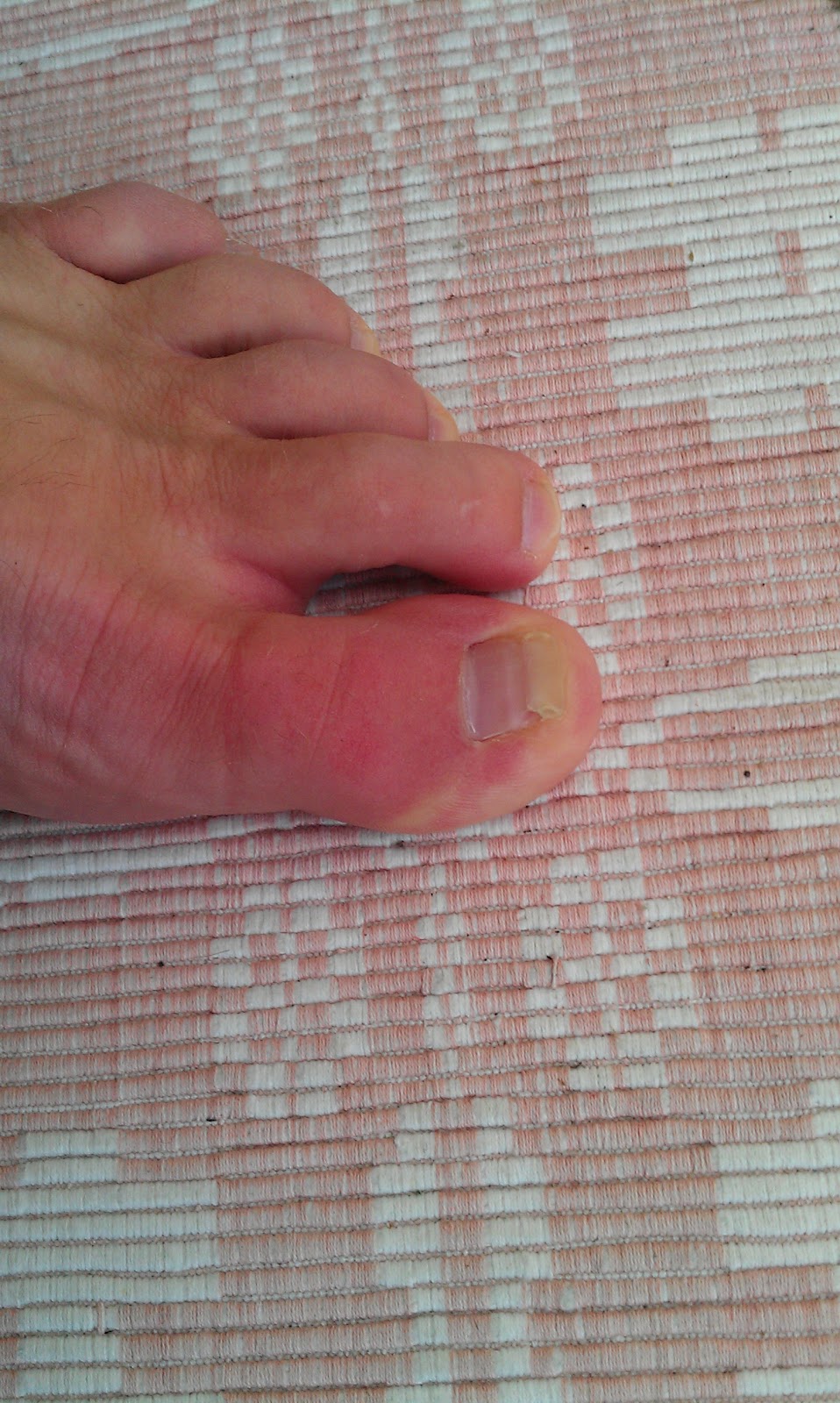
Overview
Hammer, claw, and mallet toes are toes that do not have the right shape. They may look odd or may hurt, or both. Tight shoes are the most common cause of these toe problems. A hammertoes is a toe that bends down toward the floor at the middle toe joint. It usually happens in the second toe. This causes the middle toe joint to rise up. Hammer toes often occur with bunions. Claw toe often happens in the four smaller toes at the same time. The toes bend up at the joints where the toes and the foot meet. They bend down at both the middle joints and at the joints nearest the tip of the toes. This causes the toes to curl down toward the floor. A mallet toe often happens to the second toe, but it may happen in the other toes as well. The toe bends down at the joint closest to the tip of the toe.
Causes
While most cases of Hammer toes hammertoes are caused by an underying muscle imbalance, it may develop as a result of several different causes, including arthritis, a hereditary condition, an injury, or ill-fitting shoes. In some cases, patients develop hammertoes after wearing shoes or stockings that are too tight for long periods of time. These patients usually develop hammertoes in both feet.
Some people never have troubles with hammer toes. In fact, some people don't even know they have them. They can become uncomfortable, especially while wearing shoes. Many people who develop symptoms with hammer toes will develop corns, blisters and pain on the top of the toe, where it rubs against the shoe or between the toes, where it rubs against the adjacent toe. You can also develop calluses on the balls of the feet, as well as cramping, aching and an overall fatigue in the foot and leg.
Diagnosis
The treatment options vary with the type and severity of each hammer toe, although identifying the deformity early in its development is important to avoid surgery. Your podiatric physician will examine and X-ray the affected area and recommend a treatment plan specific to your condition.
Non Surgical Treatment
You can usually use over-the-counter cushions, pads, or medications to treat bunions and corns. However, if they are painful or if they have caused your toes to become deformed, your doctor may opt to surgically remove them. If you have blisters on your toes, do not pop them. Popping blisters can cause pain and infection. Use over-the-counter creams and cushions to relieve pain and keep blisters from rubbing against the inside of your shoes. Gently stretching your toes can also help relieve pain and reposition the affected toe.
Surgical Treatment
Your podiatrist may recommend a surgical procedure if your hammertoes are not helped by the conservative care methods listed above. Surgery for hammertoes is performed to help straighten your crooked toe. Your surgery will be performed in your podiatrist?s office or at a hospital, depending on the severity of your hammertoe. A metal pin is sometimes used to help your affected toe maintain its straight position during your recovery.
Hammer Toe Causes
 Overview
Overview
Hammer, claw, and mallet toes are toes that do not have the right shape. They may look odd or may hurt, or both. Tight shoes are the most common cause of these toe problems. A Hammer toes is a toe that bends down toward the floor at the middle toe joint. It usually happens in the second toe. This causes the middle toe joint to rise up. Hammer toes often occur with bunions. Claw toe often happens in the four smaller toes at the same time. The toes bend up at the joints where the toes and the foot meet. They bend down at both the middle joints and at the joints nearest the tip of the toes. This causes the toes to curl down toward the floor. A mallet toe often happens to the second toe, but it may happen in the other toes as well. The toe bends down at the joint closest to the tip of the toe.
Causes
Hammertoes are more commonly seen in women than men, due to the shoe styles women frequently wear: shoes with tight toe boxes and high heels. Genetics plays a role in some cases of hammertoes, as does trauma, infection, arthritis, and certain neurological and muscle disorders. But most cases of contracted toes are associated with various biomechanical abnormalities of the feet, such as flat feet and feet with abnormally high arches. These biomechanical abnormalities cause the muscles and tendons to be used excessively or improperly, which deforms the toes over time.
 Symptoms
Symptoms
A hammer toe may be painful, especially when irritated by a shoe. All four toe conditions may cause cramps in the toes, foot and leg due to the abnormal function of the tendons in the foot. If a mallet toe has occurred, you are likely to suffer from a corn at the end of the toe. A hammertoe may cause a corn hammertoe on the top of the toe. Infections and ulcers can also occur. In severe cases a mallet toe, trigger toe, claw toe or a hammer toe may create a downward pressure on the foot, which can result in hard skin and corns on the soles of the feet.
Diagnosis
Hammertoes are progressive, they don?t go away by themselves and usually they will get worse over time. However, not all cases are alike, some hammertoes progress more rapidly than others. Once your foot and ankle surgeon has evaluated your hammertoes, a treatment plan can be developed that is suited to your needs.
Non Surgical Treatment
Apply a commercial, nonmedicated hammertoe pad around the bony prominence of the hammertoe. This will decrease pressure on the area. Wear a shoe with a deep toe box. If the hammertoe becomes inflamed and painful, apply ice packs several times a day to reduce swelling. Avoid heels more than two inches tall. A loose-fitting pair of shoes can also help protect the foot while reducing pressure on the affected toe, making walking a little easier until a visit to your podiatrist can be arranged. It is important to remember that, while this treatment will make the hammertoe feel better, it does not cure the condition. A trip to the podiatric physician?s office will be necessary to repair the toe to allow for normal foot function. Avoid wearing shoes that are too tight or narrow. Children should have their shoes properly fitted on a regular basis, as their feet can often outgrow their shoes rapidly. See your podiatric physician if pain persists.
Surgical Treatment
Probably the most frequent procedure performed is one called a Post or an Arthroplasty. In this case a small piece of bone is removed from the joint to straighten the toe. The toe is shortened somewhat, but there is still motion within the toe post-operatively. In other cases, an Arthrodesis is performed. This involves fusing the abnormally-contracted joint. The Taylor procedure fuses only the first joint in the toe, whereas the Lambrinudi procedure fuses both joints within the toe. Toes which have had these procedures are usually perfectly straight, but they take longer to heal and don't bend afterwards. A Hibbs procedure is a transfer of the toe's long extensor tendon to the top of the metatarsal bone. The idea of this procedure is to remove the deforming cause of the hammertoes (in this case, extensor substitution), but to preserve the tendon's function in dorsifexing the foot by reattaching it to the metatarsals. Fortunately, the Gotch (or Gotch and Kreuz) procedure--the removal of the base of the toe where it attaches to the foot, is done less frequently than in years past. The problem with this procedure is that it doesn't address the problem at the level of the deformity, and it causes the toe to become destabilized, often resulting in a toe that has contracted up and back onto the top of the foot. You can even have an Implant Arthroplasty procedure, where a small, false joint is inserted into place. There are several other procedures, as well.
 Prevention
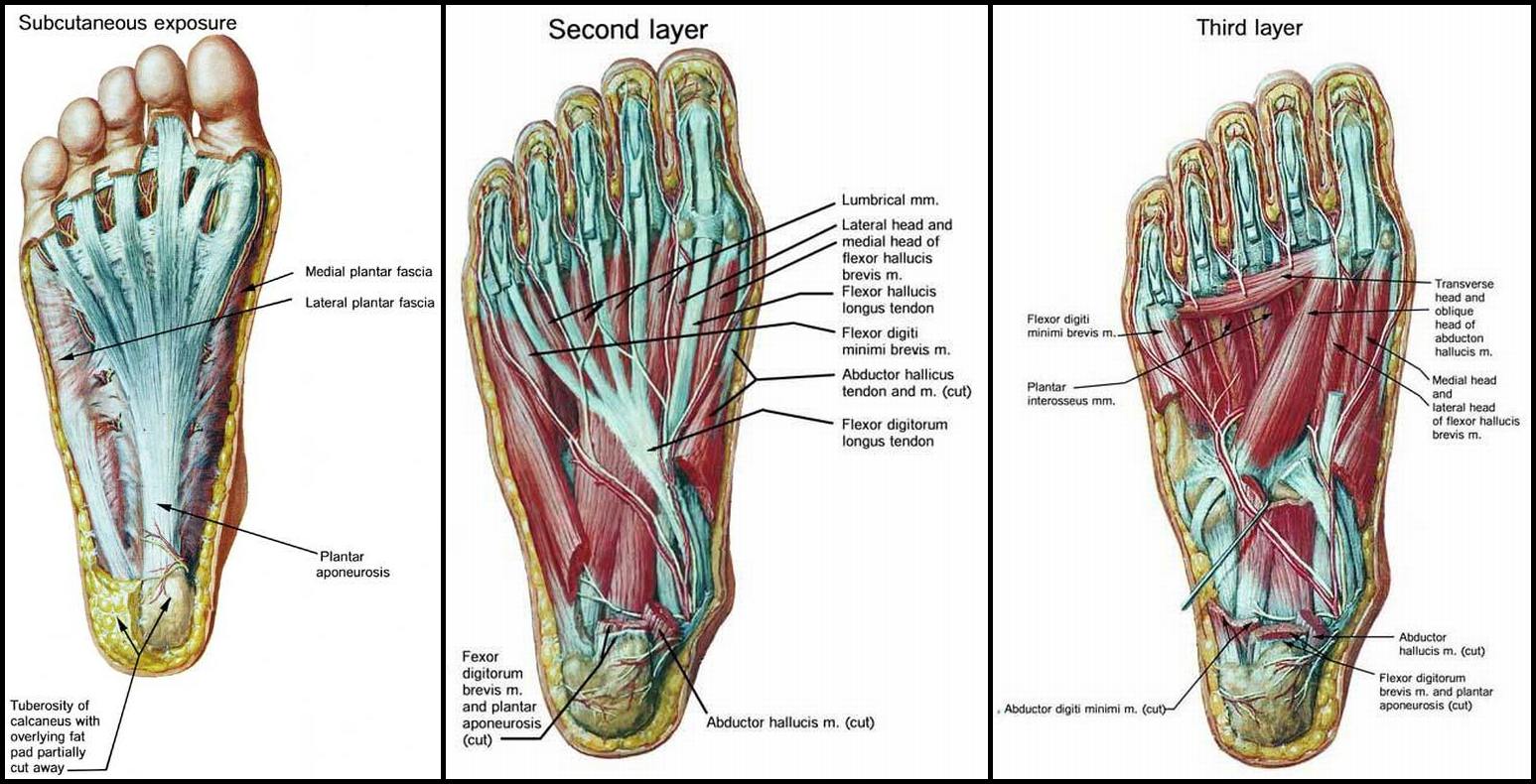
Prevention
Although these following preventative tips may be able to reverse a painful bunion or hammertoe deformity, they are more effective when applied to young people, and are less effective the longer a person has progressed with their bunion or hammertoe deformity. This is because the joints in our bodies get used to the positions they are most frequently held in, and our feet are no different, with our 12 to 15 hours a day in restrictive footwear, with tapering toeboxes, heel elevation, and toespring.
Do I Have Overpronation Of The Foot
Excessive pronation hampers our natural walking pattern, causing an imbalance and leading to wear and tear in other parts of the body, with every step we take! Whether you have a true flat foot or suffer from over-pronation in both cases your poor walking pattern may contribute to a range of different complaints. Especially with age, poor alignment of the feet will cause very common conditions such as heel pain or knee Pain.
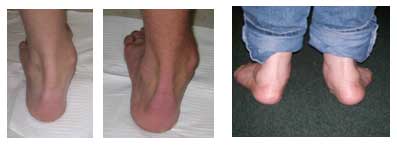
Causes
You do not have to be a runner or athlete to suffer from overpronation. Flat feet can be inherited, and many people suffer from pain on a day-to-day basis. Flat feet can also be traumatic in nature and result from tendon damage over time. Wearing shoes that do not offer enough arch support can also contribute to overpronation.
Symptoms
Over-pronation is a condition where the arch flattens out which makes the feet roll inward while walking. This condition is also known as flat feet. It imposes extreme additional stresses on the plantar fascia, a fibrous band of tissue which connects the heel to the forefoot. Over-pronation makes walking a painful experience because of the additional strain on the calves, heel and/or back. Treatment for over-pronation involves the use of specially-made orthotics which offers arch support and medial rear foot posting as corrective measures.
Diagnosis
People who overpronate have flat feet or collapsed arches. You can tell whether you overpronate by wetting your feet and standing on a dry, flat surface. If your footprint looks complete, you probably overpronate. Another way to determine whether you have this condition is to simply look at your feet when you stand. If there is no arch on the innermost part of your sole, and it touches the floor, you likely overpronate. The only way to truly know for sure, however, is to be properly diagnosed by a foot and ankle specialist.

Non Surgical Treatment
Over-Pronation can be treated conservatively (non-surgical treatments) with over-the-counter orthotics. These orthotics should be designed with appropriate arch support and medial rearfoot posting to prevent the over-pronation. Footwear should also be examined to ensure there is a proper fit. Footwear with a firm heel counter is often recommended for extra support and stability. Improperly fitting footwear can lead to additional foot problems.
Surgical Treatment
The MBA implant is small titanium device that is inserted surgically into a small opening between the bones in the hind-mid foot: the talus (ankle bone) and the calcaneus (heel bone). The implant was developed to help restore the arch by acting as a mechanical block that prevents the foot from rolling-in (pronation). In the medical literature, the success rate for relief of pain is about 65-70%. Unfortunately, about 40% of people require surgical removal of the implant due to pain.
What Are The Main Causes Of Calcaneal Apophysitis?
Severs disease (calcaneal apophysitis) is a self-limiting condition seen in physically active children. Although there is controversy about the radiographic appearance, some reports propose the importance of fragmentation of the secondary nucleus in the diagnosis of Severs disease. We studied secondary nucleus of the calcaneus with ultrasonography. Twenty-one symptomatic heels of 14 children were examined. All these heels showed fragmentation of the secondary nucleus on both conventional radiograph and sonography. Ultrasonographic examination also showed 2 retrocalcaneal bursitis. Our initial data showed that sonography may be valuable in the diagnosis of Severs disease.
Causes
There are a number of possible causes for a child's heel pain. Because diagnosis can be challenging, a foot and ankle surgeon is best qualified to determine the underlying cause of the pain and develop an effective treatment plan. Sever's disease, also known as calcaneal apophysitis, is by far the most common cause of heel pain in children. Other causes of heel pain include tendo-achilles bursitis, other overuse injuries, and fractures.
Symptoms
Symptoms include heel pain related to sports activities and worsen after those sport and exercise activities. However, some children who are not in a sport may also get this if they are physically active. If you notice that your child is ?walking on their toes? this is a sign of possible heel pain. The pain is usually on the back of the heel, the sides of the heel, the bottom of the heel, or a combination of all of these. We typically don't see swelling with this, however if pressure is applied to the sides of the heel pain may be reported. Sometimes the pain is so bad the child will have to limp, or take a break from sports activity either for a few days or few months.
Diagnosis
Your podiatrist will take a comprehensive medical history and perform a physical examination including a gait analysis. The assessment will include foot posture assessment, joint flexibility (or range of motion), biomechanical assessment of the foot, ankle and leg, foot and leg muscle strength testing, footwear assessment, school shoes and athletic footwear, gait analysis, to look for abnormalities in the way the feet move during gait, Pain provocation tests eg calcaneal squeeze test. X-rays are not usually required to diagnose Sever?s disease.
Non Surgical Treatment
If the child has a pronated foot, a flat or high arch, or another condition that increases the risk of Sever's disease, the doctor might recommend special shoe inserts, called orthotic devices, such as heel pads that cushion the heel as it strikes the ground, heel lifts that reduce strain on the Achilles tendon by raising the heel, arch supports that hold the heel in an ideal position. If a child is overweight or obese, the doctor will probably also recommend weight loss to decrease pressure on the heel. The risk of recurrence goes away on its own when foot growth is complete and the growth plate has fused to the rest of the heel bone, usually around age 15.
Exercise
For children with Sever's disease, it is important to habitually perform exercises to stretch the hamstrings, calf muscles, and the tendons on the back of the leg. Stretching should be performed 2-3 times a day. Each stretch should be performed for 20 seconds, and both legs should be stretched, even if the pain is only in one heel. Heel cups or an inner shoe heel lifts are often recommended for patient suffering from Sever's disease. Wearing running shoes with built in heel cups can also decrease the symptoms because they can help soften the impact on the heel when walking, running, or standing.
Does Posterior Tibial Tendon Dysfunction (PTTD) Always Involve Surgery Teatment ?
Overview
Adult acquired flatfoot deformity or posterior tibial tendon dysfunction is a gradual but progressive loss of ones arch. The posterior tibial muscle is a deep muscle in the back of the calf. It has a long tendon that extends from above the ankle and attaches into several sites around the arch of the foot. The muscle acts like a stirrup on the inside of the foot to help support the arch. The posterior tibial muscle stabilizes the arch and creates a rigid platform for walking and running. If the posterior tibial tendon becomes damaged or tears the arch loses its stability and as a result, collapses causing a flatfoot. Adult flatfoot deformity can occur in people of all ages and gender however, it occurs most commonly in sedentary middle aged to elderly females. There are several risk factors for posterior tibial tendon dysfunction that include: obesity, steroid use, systemic inflammatory diseases such as rheumatoid arthritis, trauma, being born with a low arch, and diabetes. It occurs most commonly in one foot however, it can occur in both feet especially in people with systemic diseases such as diabetes and rheumatoid arthritis. 
Causes
There are numerous causes of acquired adult flatfoot, including fracture or dislocation, tendon laceration, tarsal coalition, arthritis, neuroarthropathy, neurologic weakness, and iatrogenic causes. The most common cause of acquired adult flatfoot is posterior tibial tendon dysfunction.
Symptoms
The symptoms of PTTD may include pain, swelling, a flattening of the arch, and an inward rolling of the ankle. As the condition progresses, the symptoms will change. For example, when PTTD initially develops, there is pain on the inside of the foot and ankle (along the course of the tendon). In addition, the area may be red, warm, and swollen. Later, as the arch begins to flatten, there may still be pain on the inside of the foot and ankle. But at this point, the foot and toes begin to turn outward and the ankle rolls inward. As PTTD becomes more advanced, the arch flattens even more and the pain often shifts to the outside of the foot, below the ankle. The tendon has deteriorated considerably and arthritis often develops in the foot. In more severe cases, arthritis may also develop in the ankle.
Diagnosis
Looking at the patient when they stand will usually demonstrate a flatfoot deformity (marked flattening of the medial longitudinal arch). The front part of the foot (forefoot) is often splayed out to the side. This leads to the presence of a ?too many toes? sign. This sign is present when the toes can be seen from directly behind the patient. The gait is often somewhat flatfooted as the patient has the dysfunctional posterior tibial tendon can no longer stabilize the arch of the foot. The physician?s touch will often demonstrate tenderness and sometimes swelling over the inside of the ankle just below the bony prominence (the medial malleolus). There may also be pain in the outside aspect of the ankle. This pain originates from impingement or compression of two tendons between the outside ankle bone (fibula) and the heel bone (calcaneus) when the patient is standing.
Non surgical Treatment
Get treated early. There is no recommended home treatment. While in stage one of the deformity, rest, a cast, and anti-inflammatory therapy can help you find relief. This treatment is followed by creating custom-molded foot orthoses and orthopedic footwear. These customized items are critical in maintaining the stability of the foot and ankle. Once the tendon has stretched and deformity is visible, the chances of success for non-surgical treatment are significantly lower. In a small percentage of patients, total immobilization may arrest the progression of the deformity. A long-term brace known as an ankle foot orthosis is required to keep the deformity from progressing. The Richie Brace, a type of ankle foot orthosis, shows significant success as a treatment for stage two posterior tibial dysfunction. It is a sport-style brace connected to a custom corrected foot orthodic that fits into most lace-up footwear (including athletic shoes). It is also light weight and more cosmetically appealing than traditionally prescribed ankle foot orthosis. The Arizona Brace, California Brace or Gauntlet Brace may also be recommended depending on your needs. 
Surgical Treatment
If cast immobilization fails, surgery is the next alternative. Treatment goals include eliminating pain, halting deformity progression and improving mobility. Subtalar Arthroereisis, 15 minute outpatient procedure, may correct flexible flatfoot deformity (hyperpronation). The procedure involves placing an implant under the ankle joint (sinus tarsi) to prevent abnormal motion. Very little recovery time is required and it is completely reversible if necessary. Ask your Dallas foot doctor for more information about this exciting treatment possibility.